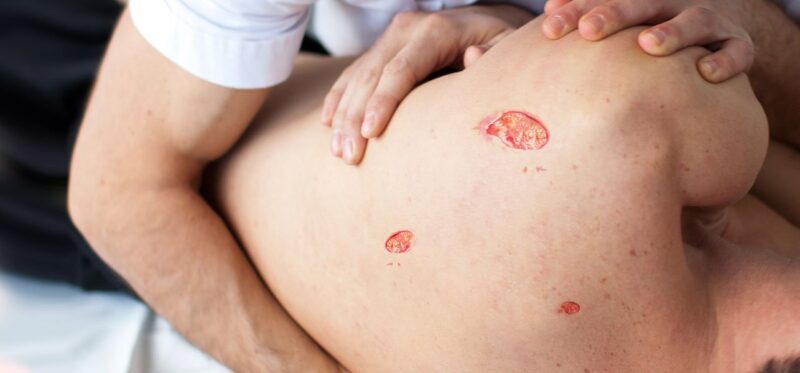
Bed sores develop on the skin of a person with limited mobility, cause pain and discomfort and infection carries and are serious risks for seniors. To prevent and treat bed sores, seniors must move around and stay in a clean environment. Caregivers must assure that the daily routines of seniors include this. Caregivers must know what causes bed sores, how to prevent them and what to do if they develop on a senior.
Causes of bed sores
Bed sores, which are also called pressure sores, are facilitated by the skin, which becomes thinner and more delicate with age. Seniors whose mobility grows limited because of disability, recovery from surgery, or fatigue may find themselves developing bedsores. For example, a senior who requires a wheelchair might find bedsores developing on the backs of their legs due to constant sitting. Seniors recovering from heart surgery need bedrest, but lying in a bed for long with no movement can cause bedsores on their backs, arms, legs or buttocks.
A bed sore looks slightly different in patients, but begin as a red, tender area on the skin. If left untreated, bed sores can split the skin and bleed, or allow germs into the skin. The resulting infection poses extreme dangers to health, causing tissue under the skin to die, affecting even the bones. (This can happen from extreme neglect, but in most cases they are caught by attentive caregivers.)
Prevention
To prevent bed sores, two procedures should be included into a routine care regimen, including checking for sores and their development and monitoring when the senior in your care spends immobile. Seniors who spend long times in bed or seated are most at risk for developing bed sores. The suggested routines require trust-building and intimacy between caregiver and the person under care. Checking for bed sores required reviewing every part of the senior’s body.
The caregiver should obtain agreement on how to check private or sensitive areas and make arrangements for a doctor to double-check, also. In addition to problems of modesty, preventing bed sores also means urging seniors to move and exercise when possible. Coordinate the plan with medical personnel to evaluate a senior’s physical capabilities. Talk to the senior about why you would like to push their physical boundaries and that it is not out of cruelty, but of care. For seniors who have limited mobility, the pain or discomfort of movement may cause them to resist such efforts. You should be sensitive to these feelings and balance them with healthcare needs.
Detection and treatment
If you care for a senior with limited temporary or permanent mobility, check regularly for bed sores. The wounds typically start small, but look raised, red, inflamed, or infected. Because skin tears more easily with age, areas with thin or sensitive skin should get checked frequently.
If an area that looks like a potential bed sore is found, contact a medical professional immediately. Most sores do not require a trip to the emergency room unless they appear severely inflamed or infected. The red flags indicating this up here in how raised or red the area is, or if it is leaking fluid of any kind. Plan to see the primary care physician promptly or go to a nearby minute clinic. Meanwhile, the senior person’s position should be changed to remove contact with the affected area. This may require extra pillows for comfort and support for a new body position.
If in one or two days the senior’s condition does not improve significantly, or if the wound shows typical signs of infection (drainage, a bad smell, or heat around the wound), the Mayo Clinic recommends seeking immediate care.
In extreme cases, bedsores may require surgery
Once treatment begins, caring for the wound involves removing damaged tissue, which should be done by a doctor, and cleaning and redressing wounds, which is typically done by a nurse but sometimes at home. It is important to heal the wound that the caregiver keep hands clean, use gloves and gauze, avoid pressure on the area during rest times, and manage the pain and discomfort. You should also discuss with a doctor familiar with the senior ways in which the senior can be supported, such as through change of diet or physical exercise routine.
In extreme cases, bed sores require intensive surgery. Although not common, it requires extensive and sometimes painful recovery. During this time preventing new sores is important because aging systems often struggle to keep up with the demands of too much healing at one time.
Sources:
Cancer Research UK. Dealing with pressure sores (sore skin). Cancer Research UK. Available at http://www.cancerresearchuk.org/about-cancer/coping-with-cancer/coping-physically/skin/managing/dealing-with-pressure-sores. Retrieved January 25, 2017.
Mayo Clinic. Bed sores. Mayo Clinic. Available at http://www.mayoclinic.org/diseases-conditions/bedsores/basics/definition/CON-20030848. Retrieved January 25, 2017.
NHSChoices. Pressure ulcers. NHS.uk, October 9, 2014. Available at http://www.nhs.uk/Conditions/Pressure-ulcers/Pages/Introduction.aspx. Retrieved January 25, 2017.